3. Improve Sperm Quality
Targeted nutrition and lifestyle changes proven to support count, concentration motility, morphology and DNA fragmentation

Welcome from Ro
Hi there – and thanks so much for being here. My name is Ro Huntriss and I’m the Founder of Fertility Dietitian UK. This article will guide you through sperm health, why it matters for fertility, and what can be done to improve it through targeted nutrition and lifestyle changes. I’ll also share how my team and I can support you on this journey. Let’s get going.
How to Improve Sperm Health for Better Fertility
When it comes to fertility, conversations often focus on egg health and female fertility, yet male factors contribute to up to half of all cases of infertility. For many men, this can come as a surprise. Fertility is rarely discussed from the male perspective, leaving many feeling overlooked, unsupported, or unsure where to begin.
It’s also common to feel overwhelmed by conflicting advice, frustrated that pregnancy hasn’t happened despite your best efforts, or uncertain about what to do next. Many men say they feel left out of fertility conversations, with little discussion around how diet and lifestyle can influence sperm health.
The good news is that sperm are continuously produced, meaning that nutrition, lifestyle, and targeted support can improve quality within a few months, with some research showing measurable improvements in as little as two weeks.
This article cuts through the confusion with clear, evidence-based steps to help you understand your results, identify what’s within your control, and take action to improve sperm health and overall fertility.
What Is Sperm Health and Why Does It Matter?
Sperm health refers to how well sperm are produced, shaped, and able to move and fertilise an egg. The process of sperm development, known as spermatogenesis, takes around 72 to 90 days, making it one of the most responsive aspects of reproductive health.
Healthy sperm rely on balanced hormones, adequate nutrients, strong cellular energy and a stable internal environment, protection from external stressors such as heat or environmental toxins. When these factors are disrupted, the number, movement, and quality of sperm can all be affected, influencing both natural conception and assisted reproductive outcomes.
Feeling stuck or frustrated after receiving less than ideal test results is common, but these numbers are not fixed. With the right approach, sperm quality can improve significantly within a few months, and in some cases even within a couple of weeks.
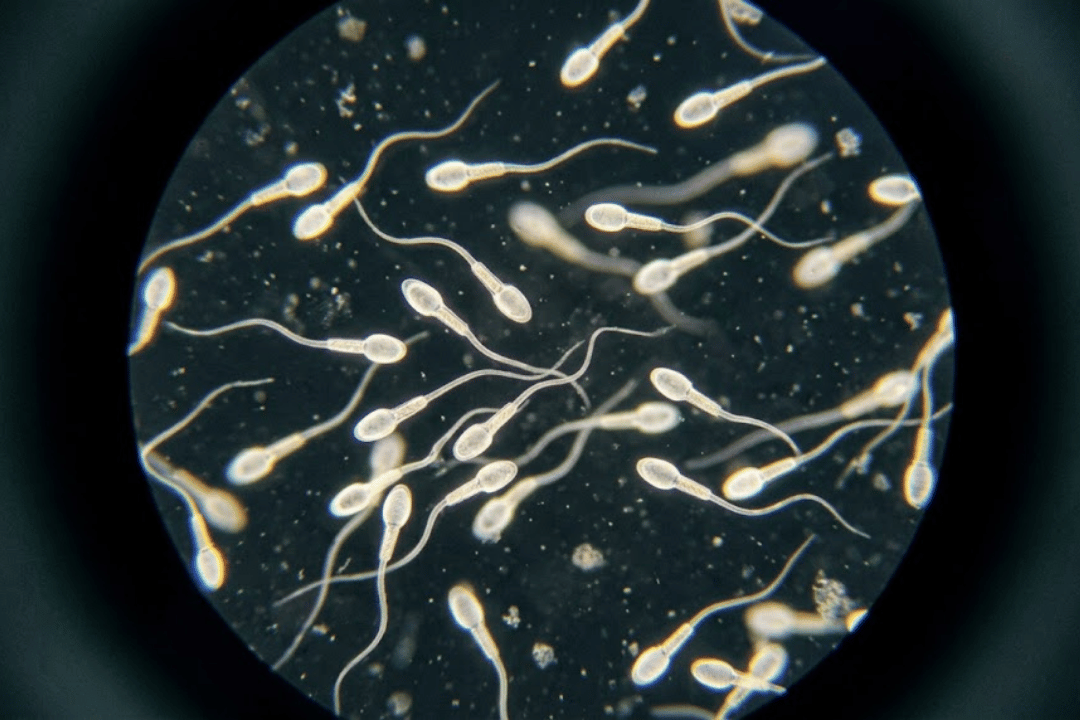
Why Sperm Health Changes
Sperm production is sensitive to internal and external influences. Oxidative stress, metabolic health, and environmental factors can all affect how well sperm develop and mature.
Common contributing factors include:
- Oxidative stress: Smoking, obesity, and poor diet increase free radical damage, reducing motility and DNA integrity.
- Nutrient status: Low levels of zinc, selenium, CoQ10, and omega-3s can impair mitochondrial function and sperm movement.
- Temperature exposure: Frequent saunas, tight clothing, or laptops on the lap can reduce sperm count and motility.
- Stress and sleep: Chronic stress raises cortisol and reduces testosterone, while poor sleep disrupts hormone balance.
- Metabolic health: Insulin resistance, excess body fat, and low testosterone can suppress sperm production.
These influences are modifiable, which means that small, consistent lifestyle changes can improve sperm function and fertility outcomes. Understanding that sperm health reflects overall wellbeing, rather than personal fault, can make these changes feel empowering rather than overwhelming.
Normal vs Optimal Sperm Parameters
The World Health Organization (WHO) reference ranges for sperm parameters are often described as “normal,” but they are based on the lower 5th percentile of men whose partners conceived within 12 months. In other words, these cut-offs represent the minimum threshold seen in a fertile population, rather than an optimal target. While they are useful for identifying clear abnormalities, they don’t define the levels associated with the best chances of conception. Research consistently shows that higher sperm count, motility and morphology are linked to improved fertility outcomes, so for men aiming to optimise their fertility, it can be beneficial to look beyond the WHO reference values rather than simply meeting them.
| Parameter | WHO “Normal” Range | Emerging “Optimal” Range (from research) |
|---|---|---|
| Semen volume | WHO “Normal” Range≥ 1.4 mL | Emerging “Optimal” Range2–5 mL |
| Sperm concentration | WHO “Normal” Range≥ 16 million/mL | Emerging “Optimal” Range> 40–50 million/mL |
| Total motility | WHO “Normal” Range≥ 42% | Emerging “Optimal” Range> 60% |
| Progressive motility | WHO “Normal” Range≥ 30% | Emerging “Optimal” Range> 50% |
| Morphology (normal forms) | WHO “Normal” Range≥ 4% | Emerging “Optimal” Range> 8–14% |
| DNA fragmentation index (DFI) (non-WHO range) | WHO “Normal” RangeVaries by assay; many labs use < 30% as favourable | Emerging “Optimal” Range≤ 15% is often considered low and associated with better outcomes |

Can You Improve Sperm Quality?
Yes. While genetics and age play a role, most of the factors that influence sperm health are modifiable. Because sperm develop in cycles of around three months, changes to diet, lifestyle, and supplement use can make measurable improvements.
If you feel frustrated that your efforts have not yet paid off, or anxious that time is slipping away, know that sperm health responds well to evidence-based changes. It is one of the most adaptable areas of fertility.
Supporting sperm health starts with addressing oxidative stress, hormone balance, nutrient status, environmental factors such as heat or toxins and overall metabolic health.
Nutrition and Lifestyle Strategies to Support Sperm Health
Supporting sperm health is not about quick fixes but about creating a stable internal environment that allows healthy sperm to develop. Consistency is key.
Foundations for better sperm health include:
- Eating a balanced, anti-inflammatory diet rich in oily fish, colourful vegetables, wholegrains, nuts, and seeds.
- Prioritising adequate sleep (7–8 hours) to support testosterone and sperm production.
- Engaging in regular physical activity and moderate exercise to improve circulation and hormone regulation.
- Reducing alcohol intake and smoking, both of which are linked to DNA damage and lower motility.
- Supporting a healthy weight, as even small reductions can enhance testosterone and sperm count.
- Managing stress, as high cortisol levels can interfere with hormone production and sperm development.

- Including antioxidant-rich foods and key nutrients known to help protect sperm from oxidative stress and support mitochondrial energy production.
- Minimising exposure to environmental toxins and excessive heat (for example, from saunas, hot tubs, or laptops on the lap), which can impair motility and sperm count.
These are just some of the strategies that can make a meaningful difference to sperm health and overall fertility.
If you want to target specific sperm parameters, there are evidence-based nutritional strategies designed to improve each sperm parameter and we go into this in detail in our Male Fertility & Sperm Health Guide or within our consultations.
Finding the Right Support
Feeling uncertain, dismissed, or overwhelmed during your fertility journey is common – and many men feel especially excluded from these conversations. If you’ve been told your sperm results are “fine,” yet conception still hasn’t happened, or you’ve been left wondering what you can actually do, you’re not alone.
Working with a registered fertility dietitian or nutritionist trained in fertility nutrition can help you:
- Cut through the confusion and identify clear, evidence-based next steps
- Build a personalised plan that supports sperm health, hormone balance, and overall fertility outcomes
- See improvements in specific sperm parameters
- Feel supported and understood throughout your fertility journey
Whether you’re preparing for IVF or ICSI, recovering from a failed cycle, or simply want to optimise sperm quality before trying to conceive naturally, we offer practical, science-backed strategies designed to support male fertility at every stage.

Our services are designed to meet you wherever you are in your fertility journey
Sperm Quality
Guide and Meal Plan
An affordable, science-backed roadmap to improving male fertility and sperm health, with a focus on proven strategies for individual sperm parameters and overall male fertility.
121 Fertility Nutrition Consultations
Personalised support with a certified specialist, to generate a personalised action plan to enable you to reach your fertility goals.
Membership Waitlist
Your complete online resource for evidence-based fertility nutrition and lifestyle support, anytime you need it.
With the right support, you can feel informed, empowered, and confident in the choices you make to improve your fertility outcomes.
References
1. de Ligny W., et al. (2025). Antioxidant Treatment and the Chance to Conceive in Men Seeking Fertility Care. JAMA Network Open.
2. Steiner A. Z., et al. (2020). Effect of antioxidants on male factor infertility: The MOXI randomized clinical trial. Fertility and Sterility, 113(3), 552–560.
3. Agarwal A., Majzoub A., Baskaran S., et al. (2022). Role of oxidative stress in male infertility and the effect of antioxidants. Reproductive Biology and Endocrinology, 20(1),
4. Majzoub A., & Agarwal A. (2021). Optimal versus normal sperm parameters: clinical implications for fertility. Andrology, 9(6), 1702–1711.
5. Skoracka K., et al. (2020). Diet and Nutritional Factors in Male (In)fertility. Nutrients, 12(5), 1400.
6. Salas-Huetos A., Bulló M., & Salas-Salvadó J. (2021). Diet, oxidative stress and male fertility: new insights. Trends in Endocrinology & Metabolism, 32(11), 882–895.
7. World Health Organization. (2021). WHO Laboratory Manual for the Examination and Processing of Human Semen (6th edition).